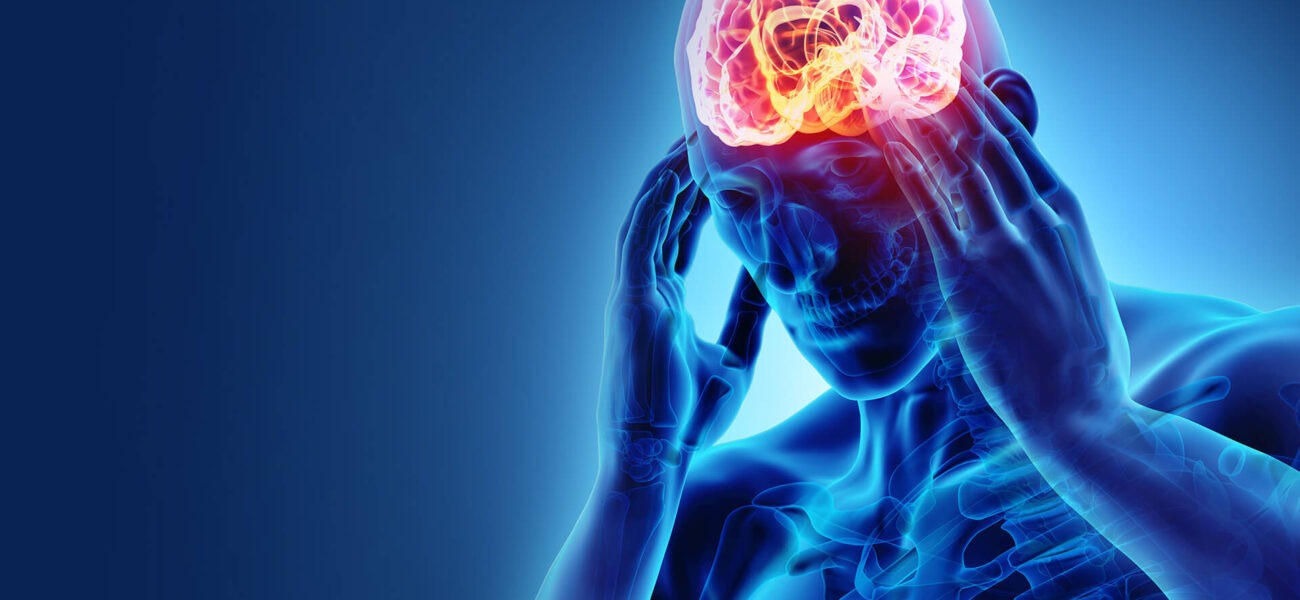
Headaches are a common problem that affects many people at some point in their lives. They can cause pain and discomfort in the head, face, or neck, and sometimes interfere with daily activities. But not all headaches are the same There are several varieties of headaches, each with its own set of symptoms, causes, and remedies. In this blog post, we will explore some of the most common types of headaches and how to manage them effectively.
What are Headaches?
A headache is a pain in your head or face that can be described in different ways, such as throbbing, constant, sharp, or dull. Headaches can vary in how severe they are, where they occur, and how often they happen. Headaches are not a disease by themselves, but they can be a symptom of another condition or a result of certain factors.
There are basically two kinds of headaches: primary and secondary. Primary headaches are not caused by another condition; they are the condition itself. Examples of primary headaches include tension headaches, migraine headaches, cluster headaches, and exertion headaches. Secondary headaches are caused by an underlying condition or situation, such as sinus infection, head injury, medication overuse, or caffeine withdrawal.
Common Types of Headaches
Some of the most common types of headaches are:
• Tension headaches are the most prevalent form of headache in adults and adolescents. They are usually caused by stress, anxiety, depression, or poor posture. They feel like a dull, constant pain or pressure on both sides of the head or around the forehead. They may also induce neck and shoulder muscular discomfort. Tension headaches typically last from 30 minutes to several hours, but they can also be chronic and occur more than 15 days a month.
• Migraine headaches: These are a type of primary headache that involves intense throbbing or pulsing pain on one side of the head. They can range from four hours to three days and occur one to four times every month on average. Migraines are often accompanied by other symptoms, such as sensitivity to light, noise, or smells; nausea or vomiting; loss of appetite; and stomach or abdominal pain. Some people also experience an aura before the headache starts, which is a visual or sensory disturbance that lasts for 5 to 60 minutes and may include seeing flashes of light, zigzag lines, or blind spots; feeling numbness, tingling, or weakness; or having difficulty speaking or finding words.
• Cluster headaches: These are a type of primary headache that cause severe burning or piercing pain behind or around one eye. They are called cluster headaches because they tend to occur in groups of one to three attacks per day for two weeks to three months. Each attack can last from 15 minutes to three hours and may be accompanied by other symptoms on the same side of the face as the pain, such as drooping eyelid, redness or tearing of the eye, runny or stuffy nose, sweating, flushing, or pupil constriction. Cluster headaches are more common in men than women and often occur at night.
Less Common Headaches
Some other types of headaches that are less common but still important to know about are:
• Sinus headaches: These headaches are caused by inflammation or infection of the sinuses (air-filled cavities in the skull). They cause pain and pressure in the forehead, cheeks, or nose, along with nasal congestion, fever, and a reduced sense of smell. They can be treated with antibiotics, decongestants, antihistamines, or nasal irrigation.
• Caffeine-related headaches: These headaches are caused by consuming too much caffeine (more than 400 milligrams per day) or withdrawing from caffeine after regular use. They cause dull, throbbing pain that may affect both sides of the head. They can be prevented by limiting caffeine intake and avoiding sudden changes in consumption. Over-the-counter pain medications can be used to treat them. hydration, and rest.
• Medication-overuse headaches: These headaches are caused by using too much pain medication (more than 10 days per month) for a long time. They cause dull, constant pain that may worsen over time and become resistant to treatment. They can be prevented by following your doctor’s instructions on how much and how often to take pain medication. They can be treated by stopping or reducing the use of pain medication under your doctor’s supervision.
• Exertion headaches: These headaches are caused by physical activity that increases blood pressure, such as running, lifting weights, or having sex. They cause throbbing pain that lasts from a few minutes to several hours. They can be prevented by warming up before exercise, staying hydrated, and avoiding extreme heat or cold. Over-the-counter pain medications can be used to treat them, ice packs, or rest.
• Hypnic headaches: These headaches are caused by unknown factors that occur during sleep. They cause moderate to severe pain that wakes you up at night, usually between 1 a.m. and 3 a.m. They typically last from 15 minutes to four hours and may recur nightly for weeks or months. They can be prevented by taking caffeine before bedtime (if your doctor approves) or melatonin (a hormone). They can be addressed with over-the-counter pain medications, caffeine pills, or lithium (a mood stabilizer).
What Causes Headaches?
The exact cause of headaches is not always clear, However, several things may contribute to them.
such as:
• Genetic factors: Some people may inherit a tendency to develop certain types of headaches, such as migraines or cluster headaches.
• Hormonal factors: Changes in hormone levels during menstruation, pregnancy, menopause, or oral contraceptive use may trigger some types of headaches, especially migraines.
• Environmental factors: Exposure to certain stimuli, such as bright lights, loud noises, strong smells, weather changes, or high altitudes may trigger some types of headaches.
• Behavioral factors: Certain habits or behaviors may trigger or worsen some types of headaches, such as stress, lack of sleep, poor posture, skipping meals, alcohol consumption, smoking, or caffeine intake.
• Medical factors: Some medical conditions may cause secondary headaches as a symptom or complication, such as sinus infection, head injury, brain tumor, stroke, aneurysm, meningitis, or glaucoma.
Getting a Diagnosis
If you have frequent or severe headaches that interfere with your daily life or if you have any warning signs that indicate a serious condition (such as the sudden onset of pain or neurological symptoms), You should speak with your doctor to get a diagnosis. Your physician will talk to you about your past medical conditions. and symptoms and perform a physical examination. They may also order some tests to rule out any underlying conditions that may cause your headache.
These tests may include:
• Blood tests: To check for infections, inflammation, anemia, or other abnormalities.
• Imaging tests: To look for tumors, bleeding, clots, infections, or structural problems in your brain or sinuses.
These examinations may involve a computed tomography (CT) scan.
or magnetic resonance imaging (MRI).
• A lumbar puncture is used to obtain cerebrospinal fluid (CSF).
from your lower back and test it for infections bleeding or increased pressure in your brain.
This test may also be called a spinal tap.
Your doctor will prescribe you the appropriate medication or refer you to a specialist depending on your diagnosis.
Some specialists who treat different types of headaches include:
• Neurologist: A doctor who specializes in treating diseases of the nervous system
which includes the brain
the spinal cord
and the nerves.
• Otolaryngologist: A doctor who specializes in ear ailments, nose, and throat.
• Dentist: A doctor who specializes in treating diseases of the teeth, gums, and mouth.
• Psychologist: A professional who specializes in treating mental health issues
such as:
• stress
• anxiety
• depression
• or trauma.
How Are Headaches Treated?
The treatment of headaches depends on the type, cause, severity, and frequency of the headache as well as your personal preferences and medical history.
Some general principles for treating headaches include:
• Identifying and avoiding triggers: You can keep a headache diary to record when your headache occurs
how long it lasts, what you were doing before it started, what you ate or drank, and what medications you took.
This can help you identify any patterns or triggers that may cause your headache and avoid them in the future.
• Taking medications as prescribed: You can take over-the-counter pain relievers such as ibuprofen acetaminophen aspirin naproxen for mild to moderate headache pain unless your doctor advises otherwise.
You should follow the dosage instructions carefully and not exceed the recommended amount or duration of use.
You should also consult your doctor before taking any prescription drugs such as triptans ergotamine anti-nausea drugs preventive drugs or opioids for your headache as they may have side effects interactions contraindications or addiction potential.
• You should also inform your doctor about any other medications supplements vitamins herbs or alternative therapies you are using as they may affect your headache treatment.
Using non-pharmacological therapies: You can also try some non-drug therapies to prevent or relieve your headache
such as:
• Applying cold or hot compresses to your head or neck.
• Massaging your head neck shoulders or temples.
• Practicing relaxation techniques such as deep breathing meditation yoga tai chi biofeedback acupuncture aromatherapy hypnosis cognitive behavioral therapy (CBT).
• Exercising regularly but moderately.