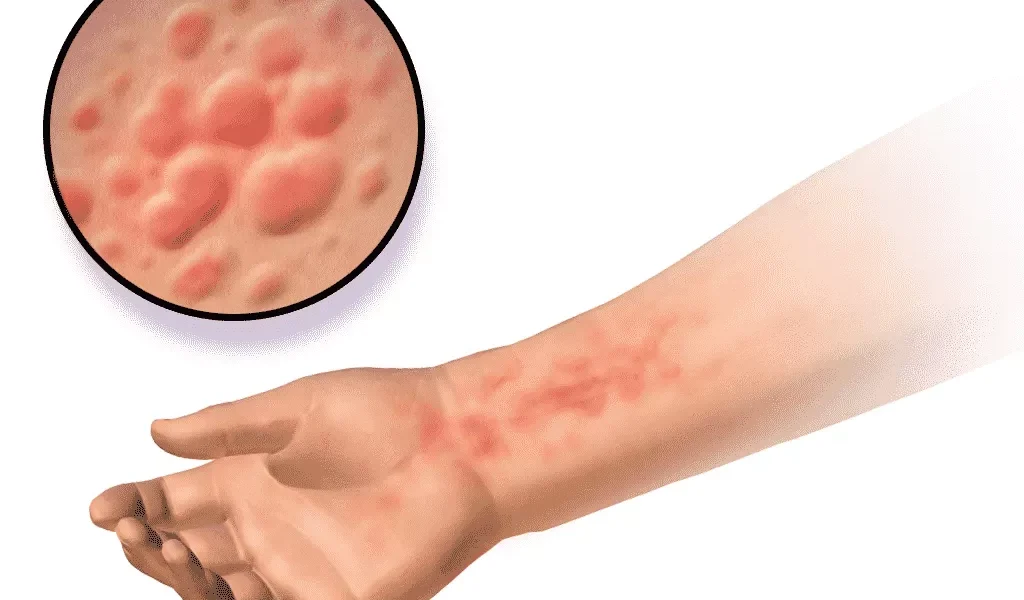
Hives, also known as urticaria, are a common skin condition that affects many people at some point in their lives. Hives are red, itchy, raised bumps or welts that appear on the skin. They can vary in size, shape, and location. They can appear anywhere on the body but are more common on the face, neck, chest, and arms. Hives can occur as a single episode or recur frequently.
Hives are usually caused by an allergic reaction to something that you have eaten, touched, or inhaled. When you have an allergic reaction, your immune system releases chemicals called histamines that cause inflammation and itching in your skin. Hives can also be triggered by other factors such as stress, heat, cold, exercise, infections, or medications.
Hives are not contagious and usually harmless. However, they can be very uncomfortable and interfere with your daily activities. In some cases, hives can be a sign of a serious allergic reaction called anaphylaxis that requires immediate medical attention.
In this blog post, we will explain the causes, symptoms, diagnosis, treatment, and prevention of hives in more detail. We will also provide some tips on how to cope with hives and when to see a doctor.
Causes of Hives
Hives can be caused by a variety of factors that trigger an allergic reaction in your skin. Some of the common causes are:
• Foods: Some foods that can cause hives are nuts, shellfish, eggs, milk, wheat, soy, strawberries, and chocolate. Food additives and preservatives can also trigger hives in some people.
• Medications: Some medications that can cause hives are antibiotics, aspirin, ibuprofen, blood pressure drugs, and codeine. You may also develop hives if you are allergic to the ingredients or the coating of some pills.
• Insect bites or stings: Some insects that can cause hives are bees, wasps, hornets, fire ants, and mosquitoes. You may also develop hives if you are allergic to the venom or saliva of these insects.
• Pollen: Some people may develop hives if they are allergic to pollen from trees, grasses, or weeds. Pollen can also be carried by insects or animals and cause hives when you touch them.
• Animal dander: Some people may develop hives if they are allergic to the fur, feathers, or saliva of animals such as cats, dogs, birds, or rodents.
• Latex: Some people may develop hives if they are allergic to latex products such as gloves, balloons, or condoms.
• Cosmetics: Some people may develop hives if they are allergic to the ingredients or fragrances of cosmetics such as makeup, shampoo, or lotion.
• Chemicals: Some people may develop hives if they are exposed to chemicals such as detergents, bleach, or paint.
Non-allergic reasons that might produce hives include:
• Stress: Emotional stress can trigger the release of histamines in your body and cause hives.
• Heat or cold: Exposure to extreme temperatures can cause your blood vessels to dilate or constrict and cause hives.
• Sunlight: Exposure to sunlight can cause your skin to produce histamines and cause hives.
• Exercise: Physical activity can increase your body temperature and blood flow and cause hives.
• Infections: Viral or bacterial infections can stimulate your immune system and cause hives.
• Chronic conditions: Some chronic conditions such as thyroid disease, lupus, or cancer can cause hives.
Sometimes the exact cause of hives cannot be identified. This is called idiopathic urticaria.
Symptoms of Hives
The main symptom of hives is the appearance of red, itchy bumps or welts on the skin. They might be as little as a few millimeters or as large as several centimeters. They can appear anywhere on the body but are more common on the face, neck, chest, and arms. They can change shape and location over time. They usually last for a few hours to a few days but can sometimes persist for weeks or months.
Other symptoms of hives may include:
• Swelling: Hives can cause swelling of the skin around the eyes, lips, tongue, or throat. This is called angioedema and can affect your breathing or swallowing.
• Pain: Hives can cause burning or stinging sensations in the affected areas.
• Fever: Hives can be accompanied by a low-grade fever if they are caused by an infection.
• Anaphylaxis: Hives can be a sign of a severe allergic reaction called anaphylaxis that involves other symptoms such as difficulty breathing, wheezing, chest pain, palpitations, dizziness, nausea, vomiting, diarrhea, or loss of consciousness.
Anaphylaxis is a medical emergency that requires immediate treatment with epinephrine (adrenaline) injections and hospitalization. Diagnosis of Hives If you have symptoms of hives that do not go away within a few days or recur frequently, you should see your doctor for a diagnosis. Your doctor will ask you about your medical history, medications, allergies, and possible triggers for your hives. They will also examine your skin and look for signs of infection or inflammation. Your doctor may also perform some tests to determine the cause and severity of your hives. Some of the tests are:
• Skin tests: These involve applying small amounts of allergens (such as foods, medications, or insect venoms) to your skin and observing for any reactions. Skin tests can help identify what you are allergic to and guide your treatment plan.
• Blood tests: These involve taking a sample of your blood and testing it for signs of infection, inflammation, or immune system disorders. Blood tests can help rule out any underlying conditions that may cause hives.
• Biopsy: This involves taking a small piece of your skin tissue and examining it under a microscope. Biopsy can help confirm the diagnosis of hives and rule out any other skin diseases.
Treatment of Hives
The best treatment for hives is to avoid the trigger that causes them. However, this is not always possible or easy to identify. Therefore, other treatments may be needed to relieve the symptoms and prevent complications.
Some of the treatments for hives are:
• Antihistamines: These are medications that block the effects of histamines in your body and reduce itching, swelling, and inflammation. Antihistamines can be taken orally (such as cetirizine [Zyrtec], loratadine [Claritin], or fexofenadine [Allegra]) or applied topically (such as diphenhydramine [Benadryl] cream). Antihistamines can help treat mild to moderate cases of acute or chronic hives.
• Corticosteroids: These are medications that suppress your immune system and reduce inflammation. Corticosteroids can be taken orally (such as prednisone) or injected (such as methylprednisolone). Corticosteroids can help treat severe cases of acute or chronic hives that do not respond to antihistamines.
• Epinephrine: This is a medication that stimulates your heart rate and constricts your blood vessels. Epinephrine is injected into your thigh muscle using an auto-injector device (such as EpiPen). Epinephrine can help treat anaphylaxis caused by severe allergic reactions to hives.
• Other medications: These include medications that target specific pathways involved in allergic reactions (such as omalizumab [Xolair] or montelukast [Singulair]) or medications that modulate your immune system (such as cyclosporine [Neoral] or methotrexate [Trexall]). These medications can help treat chronic cases of hives that do not respond to other treatments.
Prevention of Hives
The best way to prevent hives is to avoid the trigger that causes them. However, this is not always possible or easy to identify. Therefore, other preventive measures may be helpful such as:
• Keeping a diary: You can keep track of when you get hives, what you ate, touched, or inhaled before getting them, and how long they lasted. This can help you identify any patterns or potential triggers for your hives.
• Avoiding known allergens: You can avoid foods, medications, or substances that you know you are allergic to or have caused you hives before. You can also read labels carefully and ask questions before consuming anything new.
• Wearing loose clothing: You can wear clothes that do not rub against your skin or trap heat or sweat. This can help prevent physical triggers such as friction, pressure, or temperature changes from causing hives.
• Managing stress: You can practice relaxation techniques such as deep breathing, meditation, or yoga. This can help reduce emotional stress that may trigger histamine release in your body.
• Taking antihistamines prophylactically: You can take antihistamines before exposure to known allergens (such as before eating shellfish) or before situations that may trigger physical urticaria (such as before exercising). This can help prevent histamine release in your body and reduce the risk