Lung Cancer Surgery
Surgery is that the preferred treatment for patients with early stage non-small-cell carcinoma , or NSCLC. Unfortunately, most patients who have advanced or metastatic disease aren’t suitable for surgery.
People who have NSCLC that has not spread can usually tolerate surgery, provided their lungs work tolerably .
Surgery isn’t widely utilized in small-cell carcinoma (SCLC). Because SCLC spreads widely and rapidly through the body, removing it all by surgery is typically impossible. Your doctor is more likely to use treatments like chemotherapy, radiation, or immunotherapy.
What Are the kinds of Surgery for NSCLC?
In general, your surgeon removes some or all of your lung with cancer in it. The extent of removal depends on the dimensions of the cancerous tumor, where it’s , and the way far it’s spread. Your surgeon may discuss one or more of those options with you:
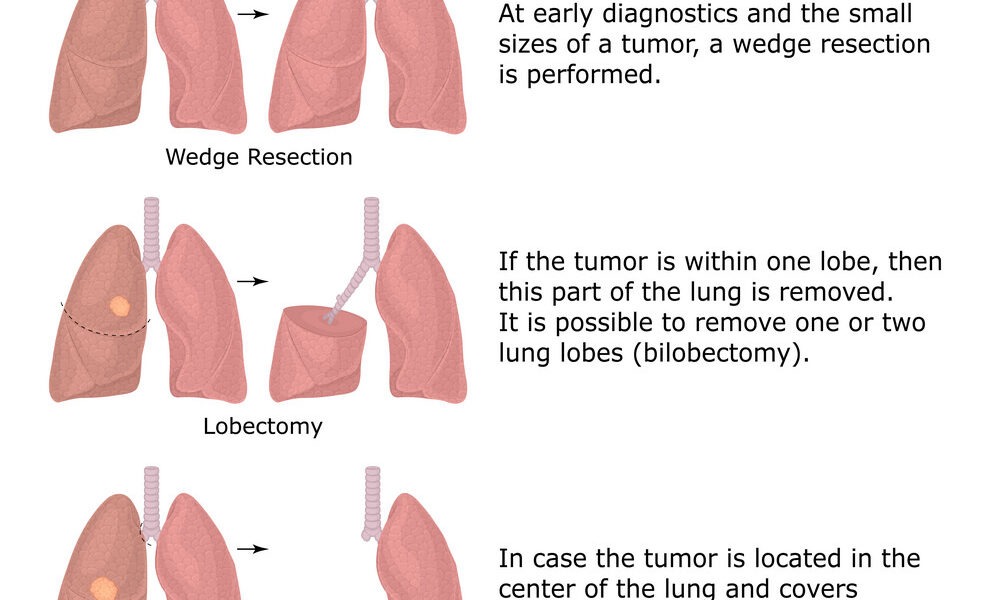
Lobectomy. Your lungs are made from parts called lobes. Your right lung has three lobes and your left lung has two. A lobectomy removes the lobe that features a cancerous tumor in it. Doctors wish to do that sort of surgery whenever possible for NSCLC.
Segmentectomy or wedge resection. These are two sorts of surgeries that remove a part of a lobe. Your surgeon might prefer to do either of them if they think removing a whole lobe would stop your lung from working well.
Pneumonectomy. Your surgeon removes the lung that has cancer in it. you’ll need this operation if your tumor is on the brink of the middle of your chest or if a lobectomy wouldn’t get obviate it.
Sleeve resection. This usually involves your surgeon removing a cancerous lobe and a part of an outsized airway called a bronchus, which matches from your windpipe into your lung. you’ve got two of those airways, one for every lung. The surgeon then attaches the most a part of the bronchus to the part that is still during a healthy lobe. they’ll do that operation rather than a pneumonectomy if they think it could assist you breathe easier.
Like all surgeries, carcinoma operations accompany risks. Ask your doctor about the possible side effects and complications of any surgery they recommend for you.
What Happens During Surgery?
Before your operation, your medical team at the hospital gives you medicine through a vein (IV) called general anaesthesia . It causes you to attend “sleep” and keeps you from feeling pain.
Once you’re unconscious, your surgeon typically uses one among two techniques to succeed in your lung:
Thoracotomy. they create an outsized cut (or “incision”) between your ribs within the side of your chest or your back.
Video-assisted thoracic surgery (VATS). they create one to four small cuts in your chest. Then they insert a small camera to ascertain images of your lung while they operate. Some surgeons do VATS by controlling a robot, which may help them make more precise movements with their surgery tools.
VATS may be a less invasive sort of surgery that’s used when possible for the treatment of early-stage NSCLC. Recovery from this sort of surgery is typically quicker than with traditional surgery.
What Happens After Surgery?
Your medical team moves you to a recovery area then to your room . They’ll keep an in depth eye on you the entire time.
When you awaken , you’ll feel groggy. Your care team will offer you medications to ease any pain. It’s common to possess tubes in your chest that your surgeon put in during the operation to empty fluid and blood — your team usually removes these after a couple of days. If you would like to travel home with a tube still in situ , your doctor or nurse will offer you instructions on the way to lookout of it.
While you’re resting within the hospital, a respiratory therapist may assist you with treatments to assist your lungs work better. they could use medications, a tool called a spirometer that tests how well you breathe, or both. you’ll ask your nurses how soon you’ll start walking again. you’ll also ask them the way to change your surgery bandages and look after your healing incision.
Before you allow the hospital, your doctor or nurse will offer you an inventory of instructions on the way to recover reception .
What if Surgery Isn’t Right for You?
Your doctor may ask you about one among these procedures for NSCLC if they rule out surgery thanks to your overall health, age, or one more reason .
Photodynamic therapy (PTD). this system uses drugs and laser light to treat early-stage lung cancers that haven’t spread beyond the outer layers of your lung airways. It also can treat tumors that block airways, helping you breathe easier.
Your doctor first gives you a drug called porfimer sodium through a vein. Then you head home and wait a few of days while the drug builds up in your cancer cells. On the day of the procedure, your doctor gives you medicines to numb your throat and relax you, or general anaesthesia to form you “sleep.” Then they insert a skinny , flexible tube with a small camera thereon , called a bronchoscope, into your nose or mouth. They guide this down your throat to the tumor in your lung. Next, a laser light on the top of the device triggers the drug within the cancer cells and destroys them. a couple of days later, your doctor uses a bronchoscope to get rid of the dead cells.
The main symptoms of lung cancer include:
A cough that doesn’t go afar after 2 or 3 weeks.
A long-standing cough that gets worse.
Chest infections that keep coming back.
Coughing up blood.
An ache or pain when respiration or coughing.
Persistent breathlessness.
Persistent tiredness or lack of energy.
The only recommended screening test for lung cancer is low-dose calculated tomography (also called a low-dose CT scan). Screening is recommended only for adults who have no symptoms but are at high risk. Screening means testing for a disease when there are no symptoms or history of that illness.